2/28/23
CanMEDS and Planetary Health: How to train a doctor
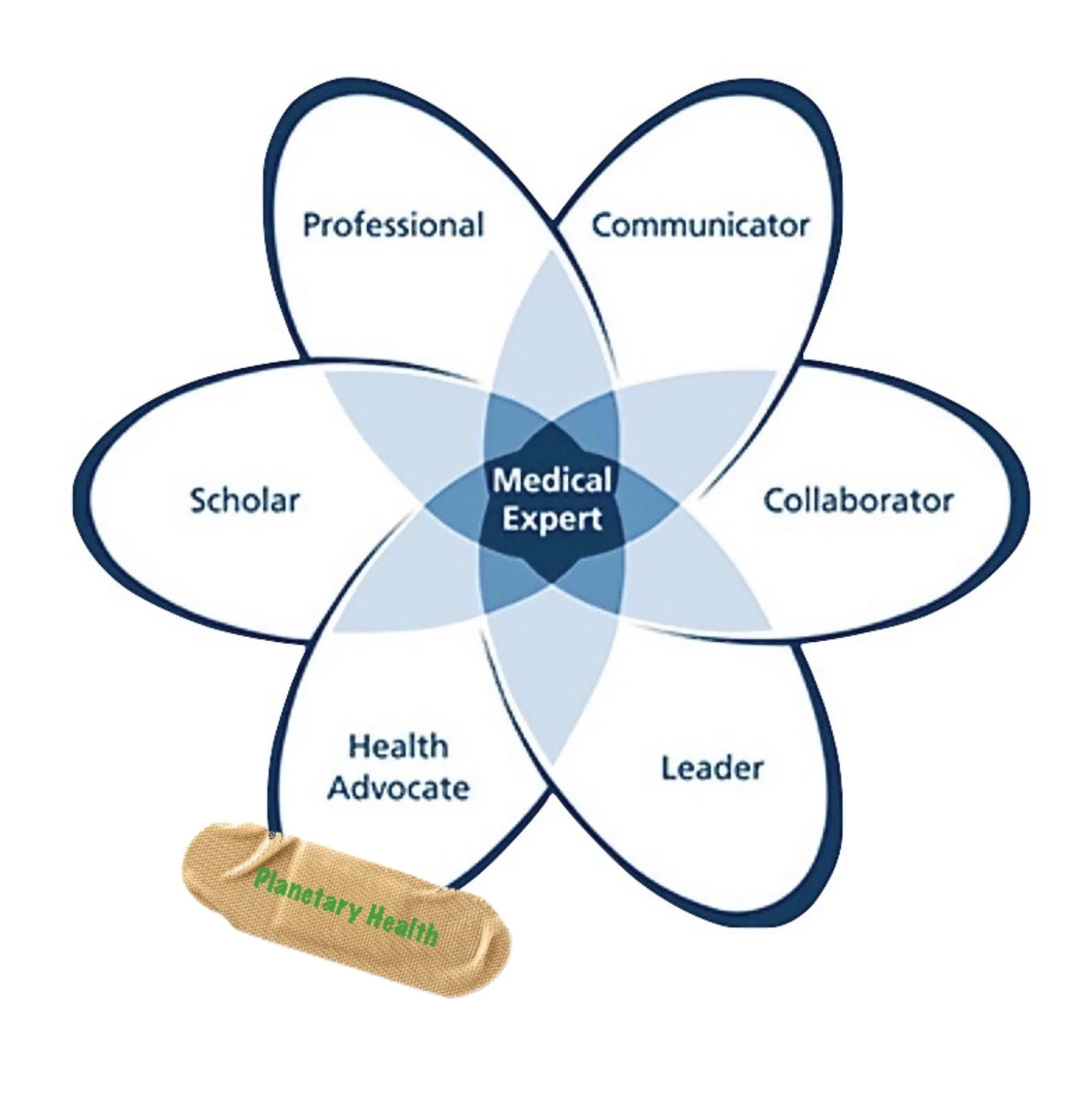
. . . although I’m obviously in favour of any efforts to educate physicians about Planetary Health, the inclusion of a lecture on the topic at a CanMEDS conference doesn’t seem quite right to me. It feels a bit like sticking a band-aid on the CanMEDS framework.
Climate criminal desflurane banished from Ontario Hospital
. . . one stands out as particularly culpable. Desflurane. If there were a carbon price on its head, this climate criminal would be dead and gone faster than it puts people to sleep.
(Originally published in The Sudbury Star on April 3, 2021)
In my last column, I shed light on the hefty carbon footprint of modern operating rooms. Much of that footprint comes from energy usage and anesthetic gases, all of which have a double life as greenhouse gases. But one stands out as particularly culpable. Desflurane. If there were a carbon price on its head, this climate criminal would be dead and gone faster than it puts people to sleep.
Desflurane, and its first-cousin Sevoflurane, are more properly called vapours. They are breathed in through a mask, and both quickly knock a person right out. I probably breathed in some gas myself two years ago for a hip replacement, and I can testify to the fact that no awareness, no pain, and no memory are really good things when you’re having major surgery.
I don’t know if I was given Desflurane or Sevoflurane. At the time, I didn’t know enough to ask. It wouldn’t have made any difference to my health, but the choice does matter to the planet’s health. Gram for gram, the two gases are not equal. Sevoflurane is 130 times as bad as carbon dioxide. Desflurane is 2540 times as bad!
Now, as promised, the big reveal. At least one hospital in Ontario has decided to get rid of Desflurane altogether, and it’s right here in Sudbury. Our very own Health Sciences North! (HSN) Leading the charge was anesthetist Dr. Sanjiv Mathur.
Mathur was exposed to the implications of climate change from a young age. His father was an IPCC scientist. So it’s ironic that he chose a specialty with a particularly high carbon footprint. Anesthetists routinely put patients to sleep with greenhouse gases, most of which are breathed back out unchanged, and dumped into the atmosphere through the roofs of hospitals.
Mathur, like many other anesthetists these days, struggled with the contradiction. In his effort to provide health care for his patients, he was causing harm to the planet’s climate and consequently to the health of all humans. This violates the best-known ethical precept in medicine: first do no harm.
In 2017, Mathur attacked the Desflurane issue head-on with a series of studies. He started by comparing the carbon footprints of Sevoflurane and Desflurane based on HSN’s purchasing records. The difference was equivalent to driving to the moon and back five times in a typical passenger vehicle.
Then he and surgeon Antonio Caycedo-Marulanda looked at 63 instances of a specific surgical procedure (called taTME) and showed that the carbon footprint of using Desflurane was forty-three times as high as with Sevoflurane. The outcomes for patients were identical.
Then Mathur looked at the carbon footprints of individual anesthetists who use Desflurane and determined that if they even cut their usage in half, they could each obliterate the carbon footprints of three to four typical Canadians each year.
After all that, he calculated that if a carbon tax were applied to these drugs, Desflurane would become so ridiculously expensive that no-one would ever use it again, which would be appropriate. It is that expensive, if we factor in the environmental costs. But we’re just not in the habit of including the health of the planet in our choices and decisions. That neglect will cost us. Escalating fires and floods, heat waves and droughts, rising oceans and melting ice are not going to be cheap, either in terms of money, or human lives and health.
Having completed their research, Mathur and Caycedo took their data and conclusions on tour, to a series of anesthesia conferences. They hope to see Desflurane eliminated altogether. However, changing physician habits is a slow way to achieve that goal.
Back home in Sudbury, HSN’s Department of Anesthesia listened to the evidence and in 2020, they decided to remove Desflurane from the hospital formulary. That means the hospital doesn’t buy it, and it’s no longer even a choice. Let’s hope other hospitals soon follow suit.
Elaine Blacklock M.D., F.R.C.P.(C)
Operating rooms have big carbon footprints too!
Help. Health. Healing. That’s what health care systems are supposed to be about. So it’s something of an oxymoron that a system intended for health is harming the health of the planet . . .
(Originally published in The Sudbury Star on Mar. 20, 2021)
When you think about our health care system, what comes to mind? Bed shortages and wait times? As a physician, I hope you also think of help. Help with maintaining your health and finding healing when sickness or injury come your way.
Help. Health. Healing. That’s what health care systems are supposed to be about. So it’s something of an oxymoron that a system intended for health is harming the health of the planet. And it’s time we face reality: people cannot stay healthy on a sick planet.
We all know that hospitals generate tonnes of garbage. But the harm I’m focusing on today is greenhouse gas (GHG) emissions. Canada’s health care system coughs out 5 percent of Canada’s total emissions, which are among the worst in the world. The American health industry is even worse: it hacks out 8-10 percent of US emissions. Health care emissions arise from many sources, like heating, cooling, and powering hospitals; doctors, nurses, and administrators driving their gas guzzlers to work; and the manufacture and transport of medical equipment, drugs, and supplies (like PPE) from as far away as China. Like everything these days, it’s complicated.
However, a few things are crystal clear. Within our health care system, hospitals are the biggest problem, and our operating rooms (ORs) are the worst offenders. Operating rooms are extravagant consumers, and they produce copious quantities of greenhouse gases and garbage. You might think that garbage and gases are an unavoidable consequence of modern health care, but some ORs manage to do the job with significantly lower emissions than others.
In 2017, Vancouver surgeon Andrea MacNeill and colleagues analysed the carbon footprints of ORs at three large hospitals, located in Vancouver, Minneapolis, and Oxford, UK. There were both similarities and some astounding differences. All three ORs had high emissions, but not necessarily for the same reasons. The biggest differences were the result of two main factors:
1) Energy: For heating, cooling, ventilation, and equipment;
2) Anesthetic gases: They help make surgery painless but they’re also nasty greenhouse gases. And among the available options, one stands out as positively nefarious. Desflurane heats up the planet some 26 times more than its first-cousin Isoflurane.
In coal-burning Oxford, 84 percent of the OR’s emissions came from energy consumption. In Vancouver, where energy comes mostly from natural gas and clean sources like hydropower, that number was only 17 percent. That’s a striking difference.
On the other hand, in the Minneapolis and Vancouver hospitals, anesthetic gases accounted for over half of OR emissions, compared with only 4 percent in Oxford. Why? The answer is simple: Oxford doesn’t use Desflurane!
Now imagine if the Oxford hospital could get rid of coal, or if Vancouver decided to banish the use of Desflurane! Either way, the result would be operating rooms with dramatically lower emissions.
Individual hospitals can try to be more energy-efficient, but they don’t have much control over where their electricity comes from. Desflurane is a different issue altogether. It’s low-hanging fruit. Easy to pluck off the tree and get rid of. Or at least it should be. Desflurane has minimal if any advantages over Isoflurane. It’s also more expensive! So why is it still in frequent use in Ontario’s operating rooms in 2021?
Here’s the main reason: It’s because physicians, administrators, governments, and patients aren’t in the habit of asking 21st century health questions, like what is the environmental impact of the equipment we’re using, the tests or treatments we’re recommending, the drugs or gases we’re prescribing??
Changing habits is a slow process. But if a carbon tax were applied to anesthetic gases, Desflurane would disappear from hospitals almost immediately. It would be unaffordable.
But I’ll finish with some good news. At least one hospital has already gotten rid of Desflurane, and it’s right here in Northern Ontario. Find out which one in my next column!
Elaine Blacklock M.D. F.R.C.P.(C)
Sources:
MacNeill, A et al. “The impact of surgery on global climate.” Lancet Planetary Health 2017; 1:e381. https://www.thelancet.com/journals/lanplh/article/PIIS2542-5196(20)30121-2/fulltext
Lenzen, M et al. “The environmental footprint of healthcare: a global assessment.” The Lancet Planetary Health. July, 2020. https://www.sciencedirect.com/science/article/pii/S2542519620301212?via%3Dihub
First, do no harm while treating asthma
. . . To put it simply, our health care is harming the planet and consequently our health . . .
(Originally published by The Sudbury Star as “Sometimes the medicine we take adds to global warming” on Mar. 6, 2021)
The phrase “First, do no harm” is a guiding principle for health professionals and researchers. It’s part of the Hippocratic Oath still sworn by graduating medical students each spring. It warns us to be very sure we aren’t harming people in the course of trying to help them.
But what should we do when the emissions that cause climate change and air pollution are harming us, actually making us sick? When the health care system we’re part of, or rely on, is producing five percent of our nation’s greenhouse gas (GHG) emissions? Or when commonly used medicines like puffers (MDIs) are responsible for some three percent of that five percent? To put it simply, our health care is harming the planet and consequently our health.
It’s a circular issue. Many air pollutants are GHGs and contribute to global heating. Many GHGs are air pollutants, which affect our health. The garbage we unthinkingly dump into our atmosphere causes more children to develop asthma and pneumonia. It also makes breathing even harder for people with other lung conditions, like chronic bronchitis and emphysema.
People who struggle to breath are often treated with puffers. I’m referring to those small little pressure canisters that propel medicines into our lungs with the squeeze of the trigger and a big breath. Puffers come in a rainbow of colours, blue, orange, red, purple . . . some for quick action to open up the airways (like salbutamol, often called Ventolin), and others to prevent or manage attacks by reducing swelling and inflammation.
There’s no question the medicines in puffers are helpful. But MDIs are basically tiny aerosol cannisters filled with chemicals that propel the medicine out in a fine breathable mist. And those chemicals are extremely potent greenhouse gases. They escape into the atmosphere where they contribute to planetary heating, both when a puffer is used, and when it’s improperly disposed of, which is most of the time. And thus, in the course of helping with a medical condition, we do harm to the planet. And when we harm the planet, we harm ourselves.
Despite their global heating effects, MDIs have been allowed because way back in the 80s and 90s, they were deemed medically necessary. But these days, there are great alternatives available for many people with asthma and other chronic lung conditions: dry powder inhalers or DPIs. DPIs are also called Turbuhalers, Accuhalers, etc. They don’t require propellants. The medication is released and inhaled by taking a sharp, deep breath. DPIs aren’t suitable for everyone, but many teens and adults can use them effectively and get the breathing help they need without making the planet hotter.
So why do MDI puffers remain so popular? Research suggests that, for the most part, it’s not an issue of effectiveness. It’s more about the prescribing habits of doctors, the inhaling habits of patients, and some cavernous holes in our drug coverage.
You may well ask: is three percent of five percent of Canada’s emissions really worth fretting about? The answer is a resounding YES! We are up against a climate change wall. We need to curtail all our emissions, as a nation, and individually.
You’ve probably heard that driving less, flying less, and eating less meat are effective ways to reduce your personal carbon footprint. A study published in the journal Thorax last year found that for people who use two puffs from an MDI each day, switching to an equivalent DPI would have the same impact on their emissions as switching from meat-eating to a plant-based diet.
If DPIs offer the same benefits as MDIs, without causing harm to the planet’s climate and consequently our health, why wouldn’t we use them? If you’re a doctor or Nurse Practitioner, revisit your prescribing habits. If you’re an MDI user, talk to your physician about less harmful options you could try.
Elaine Blacklock M.D., F.R.C.P.(C)
Sources:
Janson C et al. Carbon Footprint impact of the choice of inhalers for asthma and COPD. Thorax 2020; 75:82-84.
British Thoracic Society: Position Statement on The Environment and Lung Health 2020. Available at https://www.brit-thoracic.org.uk/about-us/position-statements/
Joshi M et al. Climate change and respiratory diseases: a 2020 perspective. Current Opinion Vol. 26:2; pages 119-127. Abstract available on-line at https://journals.lww.com/co-pulmonarymedicine/Abstract/2020/03000/Climate_change_and_respiratory_diseases__a_2020.4.aspx
Beauchesne M et al. Global initiative for Asthma report: How will new recommendations affect practice in Canada? CMAJ April 27, 2020. Available on-line at: https://www.cmaj.ca/content/192/17/E456
Wintemute K and Miller F. Dry powder inhalers are environmentally preferable to metered-dose inhalers. CMAJ July 20, 2020. Available on-line at https://www.cmaj.ca/content/192/29/E846
There’s no safe limit when it comes to air pollution
Sudburnians are all too familiar with the killing power of air pollution. Sulphur dioxide (SO2) and other toxic emissions from industry and mining killed our lakes and forests and stripped our landscape down to bare black rock . . .
(Originally published in the Sudbury Star as “Even air that’s a little dirty can be deadly” on Feb. 19, 2021
Sudburnians are all too familiar with the killing power of air pollution. Sulphur dioxide (SO2) and other toxic emissions from industry and mining killed our lakes and forests and stripped our landscape down to bare black rock. And whether we knew it or not, air pollution undoubtedly impacted the health and lifespans of the region’s human residents too.
The 1250-foot chimney known as the superstack was the 1970s solution: disperse the nastiness over a larger area so it would have less impact. Sulphur dioxide concentrations in the city immediately fell by 50 percent. Then acid rain became an international issue, and Inco became infamous as the largest single emitter of SO2 in North America. Its dirty reputation, and the imposition of tighter government regulations, finally prompted improvements in corporate behaviour and allowed the regreening of Sudbury to begin.
This July, the superstack will be replaced by two smaller stacks. The result will be a 40 percent decrease in greenhouse gas emissions, and far lower energy costs for Vale. A win-win, for sure, and just in time. Yet another new study, published last week in Environmental Health, has concluded that the health consequences of even low levels of air pollution are worse than we thought.
Researcher Karn Vohra and his colleagues focused in on one component of air pollution: particulate matter or PM2.5. These particles are so small they can fly right past the defences of our respiratory tracts and penetrate deeply into our blood streams and organs, often carrying other toxic chemicals on their backs. Even small concentrations of PM2.5 increase our risk of getting sick or dying from cancer, heart attacks, strokes, diabetes, you name it. This is not new information.
What is new are the study’s mortality estimates: in 2012, 10.2 million people around the world died prematurely from breathing PM2.5 that came specifically from fossil fuels. Just to be clear, that’s ten-point-two million premature deaths from the PM2.5 we produce as we extract and burn coal, oil, and natural gas to generate our electricity, heat our homes, cook our food, transport ourselves, and manufacture and ship our stuff around the world.
And let’s get more specific: amongst the unnecessarily dead in 2012 were 876 North American preschoolers who deserved cleaner air. Young lives cut short by lung ailments caused by the burning of fossil fuels. That’s not even taking into account all the other toxic stuff we habitually spew into the atmosphere.
But isn’t Sudbury’s air cleaner than it used to be? Indeed, it is. Air quality has improved all over Ontario, because back in 2013, we stopped burning coal to generate electricity. It was a smart move, and we are healthier for it. China, too, has done some hard work since the Beijing Olympics brought world-wide attention to the embarrassingly dense smog in their cities. They’ve help reduce the global death toll from fossil fuel PM2.5 to a mere 8.7 million in 2018. Still, that’s three-plus times the official global death toll from COVID-19, which by the way is aggravated by air pollution.
Whether you are breathing the filthy air of Delhi or the mildly polluted air of Sudbury, those tiny PM2.5 particles are affecting your life and health. And of course, PM2.5 is only one component of the brown sludge that so often hangs over our cities. Health Canada suggests that some 10,600 Canadian deaths each year can be linked to air pollution. If we had truly clean air to breath, we would live longer, healthier lives. Health care costs would decline significantly. But to make it happen, we have to stop burning fossil fuels.
And that brings us to the great climate co-benefit: If we stop burning fossil fuels for the sake of our health, we will be well on our way to halting the 21st century’s greatest health threat: climate change.
Elaine Blacklock M.D. F.R.C.P.(C)
Sources:
Good write-up on the Sudbury problem and the regreening: https://www.csmonitor.com/Environment/2020/0924/The-Sudbury-model-How-one-of-the-world-s-major-polluters-went-green
Superstack: started in 1970, operating in 1972 to disperse sulphur gases and other by-products of smelting away from the city. 1250 foot chimney
After the superstack, environmental reclamation projects began, liming and seeding, and tree planting some 300,000 trees annually.
Sulphur dioxide concentrations immediately fell by 50%
The paper I’ve discussed in abstract: https://www.sciencedirect.com/science/article/abs/pii/S0013935121000487
https://coronavirus.jhu.edu/map.html
https://www.canada.ca/en/health-canada/services/air-quality/health-effects-indoor-air-pollution.htm
Air quality trends in Sudbury, 1953-2002



